PATIENT REFERENCE
WHAT TO EXPECT
By putting compassion at the center of everything we do, we strive to deliver the best possible orthotic and prosthetic outcomes. We are here for you every step of the way.
FORMS
STATEMENT OF CERTIFYING PHYSICIAN FOR THERAPEUTIC SHOES >
PRESCRIPTION LETTER OF MEDICAL NECESSITY >
NOTICE OF PRIVACY PRACTICES FOR YANKE BIONICS, INC. >
PATIENT INFORMATION FORM >
PATIENT PACKET FOR MEDICARE DIABETIC SHOES >
QUICK LINKS
WEAR & CARE LIT >
YOUR FIRST PROSTHESIS >
YOUR DEFINITIVE PROSTHESIS >
USEFUL LINKS >


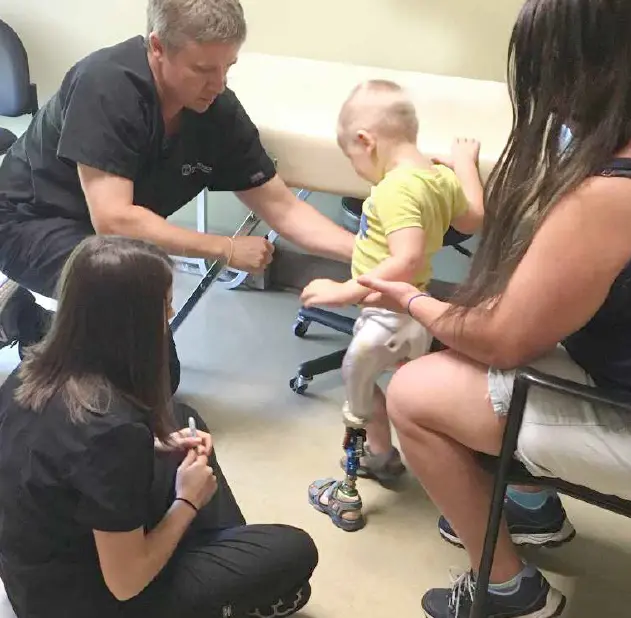
PROSTHETIC CARE: WHAT TO EXPECT
Beginning prosthetic care often comes with many questions. Experiencing limb loss can be physically and emotionally challenging, and it is normal to feel overwhelmed at different points along the way. You are not alone. Our team is here to provide guidance, education, and support throughout every stage of your prosthetic journey.
You will work with a prosthetist who will guide you through the evaluation, design, fitting, and adjustment of your prosthetic device. The level and frequency of follow up care varies based on your amputation level, healing status, activity level, and personal goals. Some patients require more frequent visits early on, while others transition to periodic check ins over time.
Your prosthetist remains involved as your needs change, helping ensure your prosthesis continues to support comfort, function, and daily life.
COMMON CAUSES OF LIMB LOSS
Limb loss can occur for many reasons. While every individual’s experience is unique, amputations most commonly result from the following:
VASCULAR CONDITIONS
Vascular disease—often related to diabetes or peripheral artery disease — is the most common cause of limb amputation. Reduced blood flow can impair healing and lead to infection or tissue damage, sometimes making amputation necessary to protect overall health. These amputations most often affect the lower limbs.
TRAUMA
Traumatic injuries, such as motor vehicle accidents, work related incidents, or severe falls, are another common cause of limb loss. Individuals who experience amputation due to trauma are often otherwise healthy and may progress efficiently through rehabilitation with appropriate prosthetic care and support.
TUMORS
Bone and soft tissue tumors may require amputation as part of treatment. Prosthetic rehabilitation can often begin once healing allows and may occur alongside other medical therapies.
CONGENITAL LIMB DIFFERENCES
Some individuals are born with limb differences due to incomplete limb development. Prosthetic care may begin early in life and is often adjusted over time to accommodate growth, activity, and functional needs.
YOUR PROSTHETIC CARE JOURNEY
Your prosthetic journey may begin before or shortly after surgery. In some cases, patients choose to meet with a prosthetist prior to surgery to better understand life after amputation and the prosthetic process.
Following surgery, your prosthetist and medical team will guide you through recovery, healing, and preparation for prosthetic fitting. Your physician will determine when you are medically ready to begin the fitting process.
Prosthetic care is a progressive journey, and most patients move through the following milestones at a pace determined by healing, readiness, and individual goals.
While this process is often described in stages, there is no one size fits all timeline. Progress is guided by individual evaluation and healing rather than fixed dates. Your care team will help determine when you are ready to move from one milestone to the next.
PROSTHETIC MILESTONES
MILESTONE 1:
RECOVERY & LIMB PROTECTION
Goal:
Protect healing tissues and establish a foundation for future prosthetic use.
Typically Includes:
- Incision and wound care
- Swelling management
- Pain control
- Proper positioning to protect joint range of motion
- Early mobility with therapy as appropriate
You are ready to move forward when your medical team confirms healing is progressing and the limb can tolerate gentle handling and compression.
MILESTONE 2:
RESIDUAL LIMB MANAGEMENT & PREPROSTHETIC REHABILITATION
Goal:
Prepare the body and residual limb for prosthetic loading and movement.
Typically Includes:
- Limb compression (such as shrinkers)
- Desensitization
- Range of motion and strengthening exercises
- Balance and mobility training
You are ready to move forward when swelling is better controlled, skin tolerance improves, and functional goals become clearer.
MILESTONE 3:
PROSTHETICE VALUATION & PLANNING
Goal:
Develop a personalized plan for your first prosthesis.
Typically Includes:
- A detailed conversation about goals and expectations
- Review of medical history and healing status
- Assessment of limb shape, skin tolerance, strength, and mobility
- Discussion of prosthetic options and components
If your limb is clinically ready, the prosthetic fitting process and insurance authorization will begin.
MILESTONE 4:
PROSTHETIC FABRICATION & DELIVERY
Goal:
Design, fabricate, and deliver a prosthesis tailored to your needs.
Typically Includes:
- Limb capture (scan or cast)
- One or more fitting appointments
- Final device delivery and initial gait or functional training
Your prosthetist will explain the expected appointment sequence and make adjustments as needed.
MILESTONE 5:
FOLLOW UP CARE & LONG TERM USE
Goal:
Optimize comfort, function, and long term success.
Typically Includes:
- Ongoing adjustments and alignment refinement
- Maintenance and component changes
- Re evaluation as activity level or health changes
Prosthetic care continues over your lifetime, and your prosthetist remains a long term resource.
UNDERSTANDING PHANTOM LIMB SENSATION & PAIN
Many people experience sensations that feel as though they are coming from the missing limb. These may include tingling, pressure, itching, warmth or cold, or the sensation that the limb is still present. These experiences are known as phantom limb sensations and are very common.
Some individuals also experience phantom limb pain, which may feel sharp, burning, aching, or cramping. This is different from normal post surgical pain and often improves over time. If symptoms interfere with daily life, treatment options are available and can be discussed with your care team.
REHABILITATION & ONGOING SUPPORT
Rehabilitation following an amputation looks different for every patient. Many individuals work with physical therapists and other healthcare providers alongside prosthetic care. Outcomes are often best when rehabilitation occurs in a coordinated, team based environment.
If there are activities you hope to return to—such as work, recreation, or sports — be sure to share those goals with your prosthetist. Your prosthetic care plan can be adjusted to support the activities that matter most to you.
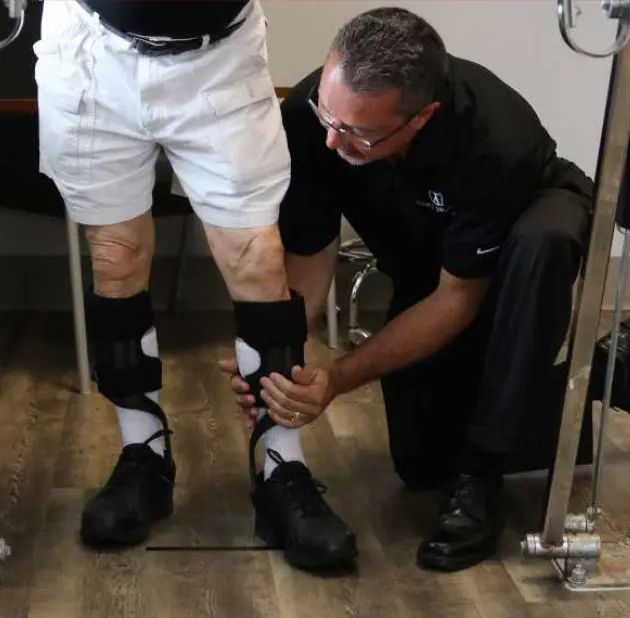
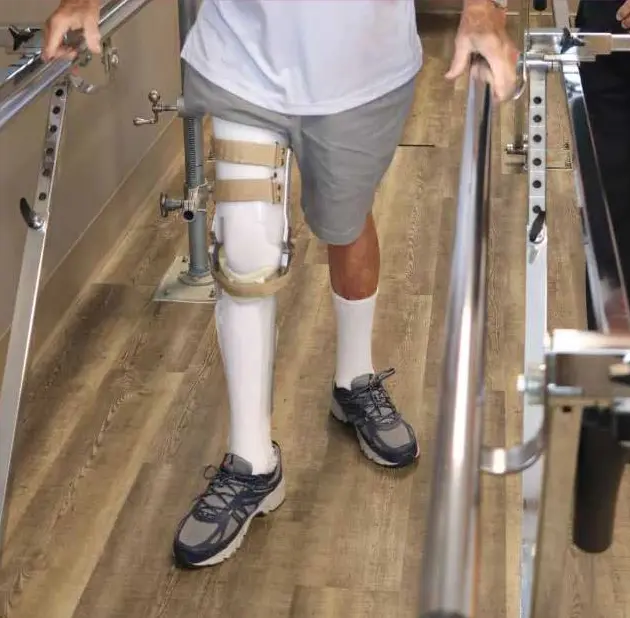

ORTHOTIC CARE: WHAT TO EXPECT
Beginning orthotic care often comes with questions — and sometimes uncertainty. Whether you are managing pain, recovering from an injury, or addressing changes in strength, alignment, or mobility, you are not alone. Our team is here to guide you through each step of the process with education, support, and clear communication.
Orthotic care is focused on supporting function, improving comfort, and helping you move with greater confidence. Your care plan is tailored to your diagnosis, activity level, and goals, and it may evolve over time as your needs change.
You will work closely with a clinician who will guide you through the evaluation, design, fitting, and adjustment of your orthotic device. Follow up care varies by diagnosis and device type. Some patients require more frequent visits early on, while others benefit from periodic check ins to ensure continued comfort, fit, and function.
Our role is ongoing. As your body, activity level, or medical condition changes, your orthotic care can be adjusted to continue supporting your daily life.
WHY SOMEONE MAY NEED AN ORTHOSIS
Orthoses are commonly prescribed to support, protect, align, or improve the function of a part of the body. A physician may recommend an orthotic device for many different reasons, including injury, chronic conditions, neurological changes, or developmental needs.
Below are some of the most common conditions and situations that may benefit from orthotic care.
MUSCULOSKELETAL CONDITIONS
Orthoses are frequently used to support joints and muscles affected by injury, wear and tear, or structural changes
Common examples include:
• Arthritis
• Tendon or ligament injuries
• Joint instability
• Overuse injuries
• Post surgical support
Orthotic devices may help reduce pain, improve alignment, limit excessive motion, or provide stability during healing and activity.
NEUROLOGICAL CONDITIONS
Neurological conditions can affect muscle strength, coordination, and control. Orthoses can help improve safety, stability, and functional movement.
Common examples include:
• Stroke • Multiple sclerosis (MS)
• Parkinson’s disease
• Traumatic brain injury (TBI)
• Spinal cord injury
Orthoses may assist with walking, standing, balance, or upper extremity function depending on individual needs.
FOOT & ANKLE CONDITIONS
Foot and ankle orthoses are commonly prescribed to address pain, alignment issues, and gait abnormalities.
Examples include:
• Plantar fasciitis
• Flat feet or high arches
• Diabetic foot conditions
• Achilles tendon issues
• Ankle instability
Custom orthotic solutions can help redistribute pressure, improve biomechanics, and support long term foot health.
PEDIATRIC & DEVELOPMENT CONDITIONS
Children may require orthotic care to support growth, alignment, and functional development.
Examples include:
• Cerebral palsy
• Developmental delays
• Toe walking
• Limb length differences
• Congenital conditions affecting movement
Orthotic care for children is often adjusted over time to accommodate growth and changing functional needs.
POST SURGICAL & REHABILITATION SUPPORT
After surgery or injury, orthoses may be prescribed to:
• Protect healing tissues
• Limit or guide movement
• Support rehabilitation goals
• Improve safety during recovery
These devices are often temporary but play a critical role in successful healing and return to activity.
YOUR ORTHOTIC CARE JOURNEY
Your orthotic journey typically begins with an evaluation by a clinician who will review your medical history, diagnosis, and functional goals. This may include a physical assessment, gait observation, and discussion of daily activities and challenges.
Based on this evaluation, your clinician will recommend an orthotic solution and explain:
• What the device is designed to do
• How and when it should be worn
• What adjustments may be needed over time
If a custom device is recommended, measurements, scans, or impressions may be taken to ensure an accurate fit.
FITTING, FOLLOWUP, AND ONGOING CARE
Once your orthosis is ready, you will return for a fitting appointment. During this visit, your clinician will:
• Ensure proper fit and alignment
• Review wear and care instructions
